Why AADC Deficiency Is Often Confused With Cerebral Palsy
Written by |

Every time doctors attempted to provide a diagnosis for our daughter, Rylae-Ann, we immediately would join the relevant support communities, start discussing things with other families, and scour the internet for interventions, only to restart the process after receiving a new diagnosis.
We had three different diagnoses in six months before discovering through genetic testing that she has aromatic L-amino acid decarboxylase (AADC) deficiency. The process of misdiagnosis is a familiar story in the AADC community, and the disease is often confused with cerebral palsy (CP).
Why the confusion?
One of the most common AADC misdiagnoses is CP, but why? AADC deficiency was first identified in 1990 by Keith Hyland and Peter Clayton. Since then, neurologists have become aware of what are known as genetic mimics of cerebral palsy. This term is used to describe how CP is comparable to several neurogenetic disorders that exhibit similar symptoms in early childhood. Genetic mimics of cerebral palsy are contributing factors to why AADC-deficient children are misdiagnosed.
Another contributing factor is that CP is a much more common movement disorder in children than AADC. Our daughter’s symptoms of dystonia (a disorder of involuntarily muscle movement), rigidity, and motor delay caused by AADC became apparent when she was about 3 to 5 months old. These similar symptoms for CP are also typically seen early on, before age 2.
A saying that is well known in the rare disease community is a phrase doctors are taught: “When you hear hoofbeats, think horses, not zebras.” This means that doctors should initially think of more common diagnoses and rule those out first before considering rare diseases.
This obviously makes sense, but you don’t want your doctors to only focus on the common diseases if you suspect they are incorrect or have a hunch it may be a rare condition. Several diagnostic tools can help to pinpoint the underlying disease and provide an accurate diagnosis.

Before being correctly diagnosed, Rylae-Ann showed signs of both hypotonia and rigidity, which also are symptoms of cerebral palsy. (Courtesy of Richard E. Poulin III)
Neuroimaging
Rylae-Ann underwent neuroimaging to determine that she did not have CP. This involved sedation and a CT scan. Later, she had an MRI, but for different reasons. Neither test showed damage or developmental changes related to CP.
These were difficult yet necessary hospital admissions. The sedation meant our daughter needed to be admitted for a few days. Her high anxiety meant screaming and crying, and when she finally woke from sedation, it took days to get her back to her ordinarily sleepy self.
Our daughter also had normal brain activity recordings from an electroencephalogram (EEG). We were even able to capture the oculogyric crises (OGC), when the muscles of the eye spasm, during an EEG. Again, the brain activity recording showed no signs that anything was amiss. It is important to note that the OGC was always a red flag for us and never matched any of the misdiagnoses we received.
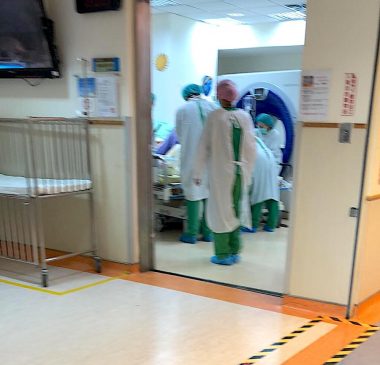
Rylae-Ann undergoes a CT scan to rule out cerebral palsy and to conduct imaging of the brain. (Courtesy of Richard E. Poulin III)
Cerebrospinal fluid
Another test our daughter underwent was her cerebrospinal fluid (CSF), which circulates through the brain and spinal cord. She had this done several times. Each time she required the medication diazepam to allow her to sleep, so she wouldn’t scream when doctors worked to extract the liquid that surrounds the spinal cord during a lumbar puncture.
Again, our daughter had to stay in the hospital and recover from the test and medication. The first time we had it done, the CSF did not alert the doctors that she had AADC deficiency, but they weren’t looking for it. The second time she underwent the test, they were explicitly checking if she had AADC deficiency, and the CSF did show it was highly likely she had it.
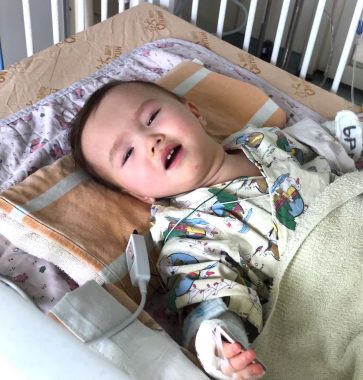
Rylae-Ann recovers after anesthesia for a lumbar puncture. (Courtesy of Richard E. Poulin III)
Future diagnosis of AADC deficiency
Diagnosis of AADC deficiency continues to improve. Newborn screening can also be performed by taking blood, giving rise to a noninvasive early detection option.
Probably the best option is yet to come. Doctors hope to analyze urine for specific levels of specific organic acids. Although this would most likely be only one of several steps, it also offers a noninvasive early detection option in the future.
I was never against testing and searching for answers. However, watching our daughter undergo invasive and extremely stressful testing that didn’t result in answers was extremely frustrating.

In the future, newborn screening could help to provide early diagnosis of AADC deficiency. (Courtesy of Richard E. Poulin III)
CP diagnosis concerns
The deficiency in neurotransmitters for AADC children results in an array of neurological and neuromuscular problems. These symptoms often mimic other more common conditions that doctors may suspect initially. Information from the observations you collect and provide your physician while also using the latest diagnostic tools can help better identify AADC deficiency in future children.
If you have concerns about a diagnosis of CP your child has received, contact your primary physician or seek a second opinion to review the diagnostic options listed above. There is even free genetic testing and counseling for families who have heard a CP diagnosis but fear another neurological condition may be involved.
Note: AADC News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of AADC News or its parent company, Bionews, and are intended to spark discussion about issues pertaining to aromatic l-amino acid decarboxylase deficiency.






Leave a comment
Fill in the required fields to post. Your email address will not be published.