The Catch-22 of Diagnostic Testing for AADC Deficiency
Written by |

Another hospital visit and another test. Searching for answers for the condition of our daughter, Rylae-Ann, meant constant hospital admissions. Between testing and treating complications of this mystery disease, the hospital staff knew us by name.
These trips involved drawing vials of blood, extracting cerebrospinal fluid (CSF), taping electrodes to her skull, and strapping her to a board while she went through a small tunnel that made loud banging noises. These were just a few of the tests she endured during our search for answers. Each time the results came back normal or inconclusive.
We wanted to complete the tests and discover the answer, but at the same time, it crushed us to see Rylae-Ann in so much pain. It was something of a Catch-22. Even taking her weight required me to hold her in a bear hug while we both got on the scale. She would arch her back and scream at the top of her lungs — the only time we saw her make such large movements.
Due to her high anxiety, we often had to sedate our daughter so the doctors could perform the tests without injury to anyone. Sedating her meant she had to stay at the hospital until she regained consciousness. However, she was still noticeably lethargic and unfocused for several days after waking.
Ultimately, the battery of tests we subjected our daughter to didn’t give us the explanation we hoped to obtain. It did help to provide data and information about what she didn’t have, but we often felt so discouraged that we didn’t even want to go to the hospital.
We ultimately discovered that she had aromatic l-amino acid decarboxylase (AADC) deficiency based on a post shared on social media. The child’s symptoms were nearly identical to our daughter’s.
Thankfully, AADC deficiency is becoming easier to diagnose. The detection methods are also becoming less invasive, which was the most challenging aspect of testing, in my opinion.
Blood test
In a video sponsored by PTC Therapeutics, Keith Hyland, PhD, explains that a blood sample can be used to measure levels of 3-O-methyldopa (3-OMD). In AADC deficiency, L-dopa is not converted to dopamine, which causes an accumulation of 3-OMD, making it “a very reliable marker for AADC deficiency.”
This testing method is less invasive for patients, as it can be performed with a simple blood draw. Instead of taking vials of blood, doctors only require a few drops, which are collected on filter paper and then analyzed.
Another positive aspect of the dried blood spot testing method is that it can be used to screen for AADC deficiency in newborns. This would guarantee an early diagnosis and determine the disease’s actual incidence rate.

A technician attaches electrodes to our daughter’s head during an electroencephalogram amid our search for answers. (Photo by Richard E. Poulin III)
Urine test
Rylae-Ann had three appointments for gene testing when we lived in Singapore. Each time, we had to go to the hospital to have vials of blood drawn. The samples were sent to a laboratory in the U.S., where the genetic test could be performed; then the results were mailed back to our doctor in Singapore. Only after scheduling an appointment to talk with our doctor did we learn the results were inconclusive.
With a simple urine test, there’s no need to send off samples. Doctors can screen patients for AADC deficiency through urinary organic acid analysis, a method already widely available at most hospitals. As AADC News’ Steve Bryson reported in 2020, the ratio of vanillactic acid to vanillylmandelic acid (both breakdown products found in urine) can help to diagnose AADC deficiency.
In the future, noninvasive urine analysis may replace invasive CSF tests as the standard method used to diagnose AADC deficiency. The testing can also be completed in house, without waiting for samples and results to be mailed back and forth.
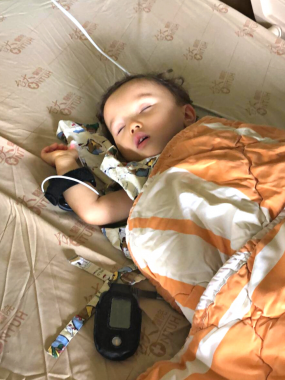
Rylae-Ann rests after several tests at the hospital. (Photo by Richard E. Poulin III)
Improving diagnosis of AADC deficiency
AADC deficiency patients in the U.S. with a confirmed diagnosis may be eligible to participate in an at-home research study by Sanguine Biosciences. According to the biotechnology company’s website, “The goal of this study is to use blood and urine samples from patients with Aromatic l-Amino Acid Decarboxylase (AADC) deficiency to help improve diagnostic testing and, ultimately, facilitate earlier recognition of the disease.”
Participants will receive $100 as compensation, and their contributions may help future children avoid being misdiagnosed or going undiagnosed for years. The study involves a technician visiting your home to collect a urine sample and take a few drops of blood. Researchers are accepting 20 participants, and my daughter is already enrolled.
Hopefully, studies like this will allow children to receive the correct diagnosis sooner and undergo less invasive testing in the future.
Note: AADC News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of AADC News or its parent company, Bionews, and are intended to spark discussion about issues pertaining to aromatic l-amino acid decarboxylase deficiency.






Leave a comment
Fill in the required fields to post. Your email address will not be published.