Preventing Aspiration After Feeding in AADC Children
Written by |

Courtesy of Richard E. Poulin III
Keeping children with AADC deficiency upright during and after feeding is important to avoid aspiration and dangerous lung infections.
Aspiration, a condition in which food or liquid enters the airway instead of the esophagus, requires our constant attention when caring for children with aromatic l-amino acid decarboxylase (AADC) deficiency. Due to the motor and autonomic dysfunctions associated with AADC deficiency, unfortunately, early death is common due to our children being at a high risk of aspirating.
When my wife first learned about AADC, we began researching potential complications and issues we should note. Our doctor alerted us to aspiration. Although we quickly learned a lot about aspiration and were diligent to prevent it, our daughter, Rylae-Ann, was still admitted to the pediatric ICU for five days due to a severe lung infection caused by aspiration.
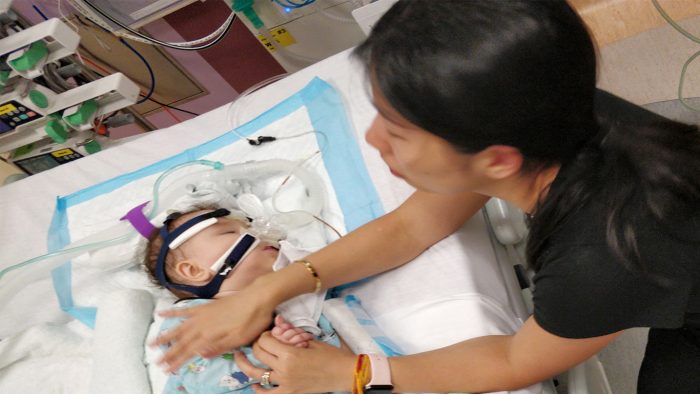
Mommy watches over Rylae-Ann in the pediatric ICU after problems with aspiration led to a severe lung infection. (Courtesy of Richard E. Poulin III)
We almost lost our daughter. So what went wrong? How did this happen? We were so careful during feedings, and provided only a liquid diet.
We didn’t realize that even though the feeding process might be over, digestion was not. Aspiration can happen during or after feeding. What we do as caregivers during feeding is just as important as what we do after it. Talking with our pediatrician, we learned two necessary steps to reduce future incidences.
30-minutes upright after feeding
Feeding is a difficult process. We were determined to keep Rylae-Ann off a feeding tube, if possible, but at the same time, we didn’t want to risk her choking. The entire digestive process relies on the coordination of several muscles that happens instinctively for typical children. However, hypotonia, or low muscle tone, affects the muscles necessary for problem-free digestion.
We invested in a comfortable highchair that came with as much support as possible. Despite being the best purchase we could find, we still needed to provide additional support with neck pillows and rolled-up towels. Feeding was still tricky, though, and she didn’t enjoy it much.

When feeding Rylae-Ann in a highchair, we added additional supports for comfort and posture. (Courtesy of Richard E. Poulin III)
We had to balance making Rylae-Ann happy while avoiding causing her to laugh while eating. Our strategy was to offer praise and positive reinforcement after each bite. If she refused, we would back off but not scold her. An iPad and music also helped to improve the environment.
When we were traveling or outside our home, supportive highchairs weren’t available. Instead, we used a baby carrier that had a hip seat attached. I found this to be a practical baby carrier when going around the neighborhood, and it also worked out well for feedings.
However, during feedings, I would put down the straps and hold her across the waist while Mom fed her. I used my chest to help keep her back upright, and between bites, we could take a tour around to keep her happy.

This style of baby carrier with a hip seat was perfect for feeding with the straps down. (Courtesy of Richard E. Poulin III)
Using the baby carrier was a great workout since feedings could easily take an hour. However, I understand that this is not the most practical way to feed. As Rylae-Ann got older, the hip seat became less of an option, but our supportive highchair remains today.
Inclined position while lying down
My wife and I were the most careful during feedings. After we were done, we kept Rylae-Ann upright, but eventually, we were drained from the feeding process. We would put her down and coo her to sleep. However, she was completely flat. I believe this was the action that led to her hospitalization.
Once we had her back home after being discharged a week later, we had already upgraded her bed with foam wedges so she could lie in an inclined position. These are inexpensive and even offer a more comfortable sleeping position. Various heights and degrees of firmness are available, making it easy to adjust for different activities throughout the day.

Rylae-Ann lies on a foam wedge pillow with the right firmness and material to keep her cool. (Courtesy of Richard E. Poulin III)
While sleeping or resting, we kept Rylae-Ann propped up at a 45-degree angle by using a standard foam firmness. Ours was made of gel memory foam, which provided the extra benefit of soothing her sweating. She would not go into this position until at least 30 minutes after eating. Some days she was exhausted, and we just let her sleep on our shoulders or use our bodies to keep her propped up.

Daddy and Rylae-Ann are exhausted but remain upright when resting. (Courtesy of Richard E. Poulin III)
We tried to keep Rylae-Ann in different positions throughout the day. We sometimes used a bouncer or a U-shaped pillow, which was Rylae-Ann’s favorite, while other times we put her in a standing position.
Another helpful device was an adjustable mesh rocker. This kept her cool while staying in a 45-degree position. It could be rocked or locked into place. The supportive mesh netting also kept her from developing a flat spot on the back of her head. This foldable rocker came with us everywhere!

Wherever we were, we kept Rylae-Ann comfortable in various upright positions. (Courtesy of Richard E. Poulin III)
Feeding AADC children
Aspiration and lung infections in AADC children are serious complications with significant risk. They usually occur as a result of a child’s inability to digest food properly. Just because your child swallows their food successfully doesn’t mean the digestion process is complete.
Even if your child uses a feeding tube, you must still be aware that aspiration is still possible. Digestion is a complicated process that can be made easier, but we must remain vigilant.
Ensure your child is in a proper position when feeding and remains upright for at least 30 minutes. After feeding, they should stay in a 45-degree position to ensure the food does not come back up. Even a minor case of aspiration can lead to serious side effects. Aspiration can lead to lung infection and hospitalization, and can even be fatal.
If your child is experiencing coughing, shallow breathing, low blood oxygen levels, and a fever, this could indicate a lung infection. Our daughter appeared pale, was wheezing, and had a cough. We thought she was sick and didn’t even realize she had a collapsed infected lung from aspirating several days prior. Visit a doctor at the first signs of trouble or if you are unsure.
***
Note: AADC News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of AADC News or its parent company, Bionews, and are intended to spark discussion about issues pertaining to aromatic l-amino acid decarboxylase deficiency.




Leave a comment
Fill in the required fields to post. Your email address will not be published.