Tips for Administering Medication to Children
Written by |

During our family’s diagnostic journey to find answers, we were prescribed various medications. After discovering that our daughter, Rylae-Ann, had aromatic l-amino acid decarboxylase (AADC) deficiency, we hoped a new set of medications would alleviate her symptoms.
But administering her medication has never been easy. Hypotonia and autonomic dysfunction mean that taking medication orally has been nearly impossible for Rylae. However, we have discovered several strategies through trial and error and by discussing the issue with other parents.
When we gave Rylae medication or supplements by mouth, she would spit it out. Sometimes, the pill would break or dissolve during her efforts to eject it from her mouth, delivering a gag-inducing bitter flavor. This would result in screaming, coughing, and usually vomiting. Giving medication became a dangerous process because we worry about complications related to aspiration.
Thankfully, we have become more successful, and the process has become much more manageable. The following tips are worth discussing with your primary care physician if your child has been prescribed oral medication or supplements.
The psychological approach
If your child is already familiar with a medication bottle or a colored tablet, keep it hidden. Prepare it stealthily and try to camouflage it. The mere sight of the bottle can trigger anxiety or negative feelings that make your task difficult. With medication, we try to be truthful and happy during the entire process and provide rewards afterward. Do your best to make it a positive experience.
You can go a step further and sneak it into their food or drink, but our physician warned us to be very cautious with that approach. AADC-deficient children are prone to being underweight due to feeding problems. If they suspect food contains medication or begin to associate the same negative feelings with meals, the medication can become counterproductive. Additionally, mixing a medicine with food or liquid may affect its efficacy. Finally, your child will need to finish the entire meal to ensure they took all of the medication. You may risk not giving a full dose.
That said, we sneak it in all the time. We have tried various foods, experimenting to see which obscures it the most.
For example, we give Rylae pyridoxal-5′-phosphate, an activated form of vitamin B6. I tasted a finger dab of the contents to see what we were up against, and I immediately gagged. We tried adding it to chocolate milk, applesauce, and oatmeal. We recently added it to ketchup of all things, and it was the most successful food yet.
However, it’s important to experiment. I think the ketchup was helpful because there was no noticeable color difference. The B6 gave her food a noticeable orange tint, and she quickly caught on to what was happening.
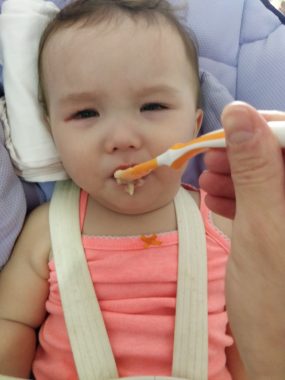
We tried hiding Rylae-Ann’s medicine in her food, but she often notices. (Courtesy of Richard E. Poulin III)
The liquid approach
Some medications are available in liquid form. Ask your doctor about your options. For some medicines, we could use a syringe or graduated dropper to drip the mixture into the back of her cheek, doing our best to bypass the taste buds. Usually, liquid medications have a sweet taste.
Unfortunately for us, the taste still didn’t satisfy our daughter’s palate. For example, we tried giving her liquid paracetamol when she had a high fever, but she immediately threw up the syrup. We tried in vain to clean a wretched red, sticky mess while also trying to make sure she didn’t aspirate.
Try to begin the process positively. Over time it’ll become easier. Aim the liquid toward the cheek and as far back in the throat as possible to reduce the likelihood of it being spat out. Some parents of children with more muscle tone than our daughter hold the cheeks together to prevent their child from spitting out the medication.
If no liquid form of the medication is available, talk to your doctor about the possibility of dissolving the medicine in water. You can then use a syringe to administer it. The pharmacist can help with dosing a crushed pill into water. We noticed that warm water not only dissolved better but also caused less sensory overload. Also, the more water we added, the less taste was detectable in the diluted mixture.

Using liquid or creating liquid medication makes administration much easier. (Courtesy of Richard E. Poulin III)
Alternative approaches
During hospitalizations, we explained to nurses that our daughter had trouble with oral medications. They were able to give some in a suppository form. Many drugs absorb very well this way, and their effects happen just as quickly, if not more so, than via the oral route.
Other medications were given intravenously or through a feeding tube during hospitalizations. After being discharged, though, we were left with the approaches mentioned above. However, our daughter received better care thanks to our requests that medication not be given orally if possible.
We are also exploring gummy versions of vitamins and supplements that will hopefully become available to pharmaceutical companies. It looks like candy and tastes like it, too. Giving gummy medication hasn’t been any trouble since Rylae developed her feeding skills. If your child is still developing this skill, you can cut the gummy up and make it a little wet so it’s slippery. It goes down almost like water.
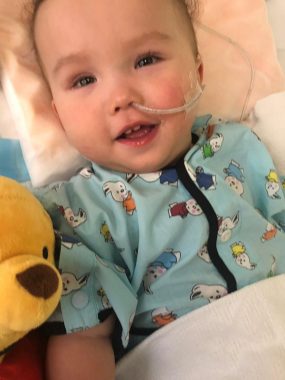
During hospitalizations, Rylae-Ann was given medication via feeding tubes. (Courtesy of Richard E. Poulin III)
Upright position
In closing, talk with your physician about the available forms of medication. Find the form that best works for you and your child at home, and advocate for it during hospitalizations. Crushing pills and dissolving them into a bitter liquid requires time and basic chemistry skills, but it makes them easier to administer. In contrast, coated tablets don’t have any flavor but are not the easiest to get children to swallow.
Regardless of the approach, always administer medication when your child is in an upright position in case of trouble. Afterward, monitor them and keep them upright for at least 30 minutes. Be sure to give your child the proper dosage, and understand what the steps are if your child vomits or spits out the medication. The protocol may be to give the medication again if you see it in the vomit or wait until the next dosage, depending on how much time has passed.

We use a supportive upright position whenever giving medication to Rylae-Ann. (Courtesy of Richard E. Poulin III)
Note: AADC News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of AADC News or its parent company, Bionews, and are intended to spark discussion about issues pertaining to aromatic l-amino acid decarboxylase deficiency.





Leave a comment
Fill in the required fields to post. Your email address will not be published.