How Pediatric Medical Traumatic Stress May Have Affected Our Family
Exploring the effects of medical trauma in children
Written by |

Our daughter’s first three years of life were spent in a hospital. The first year involved diagnostic testing and fighting to thrive due to severe symptoms of aromatic l-amino acid decarboxylase (AADC) deficiency. The second year was gene therapy, and the third was hip surgery and recovery.
Fortunately, Rylae-Ann, now 4, has since been hospital-free, but what were the effects of those three years of medical trauma?
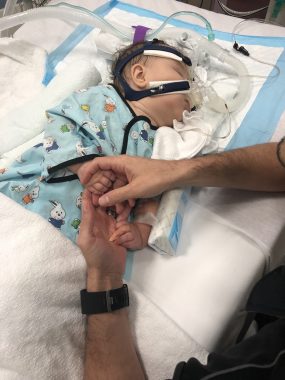
One of Rylae-Ann’s many hospitalizations due to the symptoms of AADC deficiency. (Courtesy of Richard E. Poulin III)
During a chat with our school’s counselor, I got sidetracked speaking about how my daughter has emotional outbursts beyond tantrums whenever we visit a hospital. As soon as we arrive, she arches her back and becomes rigid. With fists clenched and eyes tightly shut, she begins to scream and cry at the top of her lungs. She opens her eyes periodically to see if the nightmare is over, and we try to calm her. But in this state, it seems like she doesn’t even see or hear us, and we’re forced to restrain her as she goes through the entire process at the hospital.
The outbursts happen even if we go anywhere remotely similar, and we have to work to calm our daughter. COVID-19 protocols have caused it to happen frequently. When we go to school or even a shopping mall, we are greeted by people in medical masks holding temperature-reading tools. This causes noticeable anxiety and often screams. After a few minutes, she realizes she’s not in a hospital and relaxes.
The counselor mentioned something I’d never heard of or even considered: a condition known as pediatric medical traumatic stress (PMTS). She was becoming more aware of this disorder herself, which piqued my interest, so I started researching.
It’s wonderful to be in a position today where we can reflect on our past as we move on to the next chapter of our lives, thanks to the fantastic results of gene therapy. Without it, the medical trauma would have continued.
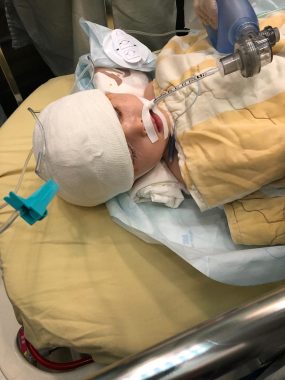
Although gene therapy provided lifesaving results, the experience was still traumatic for Rylae-Ann at 18 months old. (Courtesy of Richard E. Poulin III)
PMTS is an array of psychological and physiological responses a child or a family member experiences following medical trauma, such as pain, injury, serious illness, procedures, invasive treatment, or frightening medical experiences. It could be a single event or multiple events. For our family, it was a series of frightening and often invasive medical treatments.
According to the National Child Traumatic Stress Network (NCTSN), “Many ill or injured children and their families (up to 80%) experience some traumatic stress reactions following a life-threatening illness, injury, or painful medical procedure.” These reactions can impair daily functioning, affect adherence to medical treatment, and prevent full recovery.
The NCTSN groups the effects of medical trauma into three categories. The first is reexperiencing the traumatic event, which can take the form of flashbacks. The second is avoiding talking about or connecting with anything related to the trauma. Children may avoid hospitals, doctors, equipment, or activities surrounding the event. The third is hyperarousal, or activation of the fight-or-flight response, which occurs when the child fears for their life. It can manifest as extreme reactions.
Authors of an article published in The Journal of Child Life: Psychosocial Theory and Practice in March 2021 noted that PMTS is “a newly emerging term in the literature.” The topic is still being explored and developed, but I was constantly nodding my head in agreement as I read what information was available.
My wife and I always referred to Rylae-Ann’s outbursts as post-traumatic stress disorder as a way of explaining what we were witnessing, not realizing there was a more precise explanation. Our daughter has not been diagnosed with PMTS; regardless, it’s important to recognize that although children are young and resilient, negative experiences can have consequences.
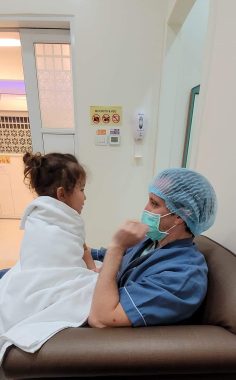
Rylae-Ann and her father talk about her hospital visits to try and calm her. (Courtesy of Richard E. Poulin III)
Moving forward, my wife and I will explore PMTS further as more research findings are reported so we can help our daughter overcome her anxiety surrounding hospitals, medical professionals, and treatment. In the meantime, we schedule telehealth appointments to fill her prescription and follow up with the doctor.
Finally, my wife and I must also consider exploring PMTS for ourselves, as we were not immune to the trauma of our daughter’s experiences. As we support Rylae-Ann, we can also help each other fully transition to the next chapter in our journey together.
Note: AADC News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of AADC News or its parent company, Bionews, and are intended to spark discussion about issues pertaining to aromatic l-amino acid decarboxylase deficiency.





Leave a comment
Fill in the required fields to post. Your email address will not be published.