Preventing Hip Dislocation in Children With AADC Deficiency
Written by |

We struggled to comprehend the news and reeled from the shock when our daughter, Rylae-Ann, was diagnosed with a rare disease known as aromatic l-amino acid decarboxylase (AADC) deficiency. We tried our best to learn about interventions and proactive steps. We concentrated on improving her eating to prevent aspiration and ensuring adequate sleep to minimize oculogyric crises. However, we neglected a vital complication, as we did not realize it was a concern.
Children with conditions that make them immobile are at risk for hip subluxation and dislocation. Due to our daughter’s immobile state, we did not even realize she had a dislocated hip. It was highly likely that the hip never formed correctly. She was not in pain, but it would require invasive surgery. After surgery, she had to wear a spica cast and undergo additional therapies.
Hip subluxation and dislocation
Hip subluxation and hip dislocation happen when the hip joint is out of its natural position. This can happen slowly, and may not look the same as a painful hip dislocation after a severe injury.
The pelvic bone has a socket joint where the ball is on the head of the femur bone. The ball can move freely within the socket, allowing the leg to move. However, when the ball is not entirely in the socket of the pelvic bone, it is called hip subluxation. This incorrect placement restricts movement and will alter the pelvic and femur bones’ shape and growth progress. Over time, without action, the subluxated hip can become fully dislocated. This is when the hip is not in the socket, which can be accompanied by pain.
Identify the dislocated hip
As Rylae-Ann grew, we noticed that one leg seemed longer than the other. We were not alarmed, as we thought it was related to her low muscle tone and paralytic state. I thought it was just her muscles being very relaxed and not strong.
We had more pressing issues such as intensive care admissions and figuring out what was going on than a slight difference in her legs. She was not in any pain, but we thought we would ask for an X-ray anyway. The doctors did not think anything was wrong, either, and were just as surprised to learn her hip was dislocated.
After identifying the dislocation, we were more aware of how differently each side of her body moved. It was barely perceptible since Rylae-Ann did not move much anyway, but the difference was there. Although our daughter did not show it, a dislocated hip may make a popping or clicking that is heard or felt.
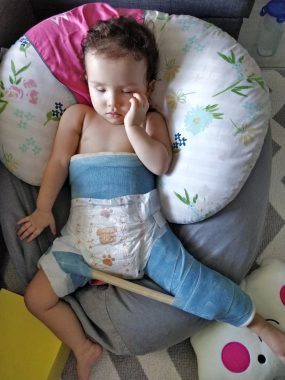
After we identified the dislocated hip, Rylae-Ann underwent open reduction hip surgery. (Courtesy of Richard E. Poulin III)
How it happened
There is not enough research dedicated specifically to AADC deficiency and how it leads to hip issues. However, we can deduce how this happens by reading literature related to other disorders with similar symptoms of hypotonia and immobility. Our thoughts were supported by the orthopedic surgeon who operated on our daughter’s hip.
It may be caused by not putting weight on the legs. As a child grows and develops, the shape of the bones changes through bearing weight (standing or walking). This helps keep the hip in its socket. If the child is not carrying weight, the hip cannot develop properly.
Another reason may be related to muscle tone and spasticity, or how muscles contract or stay tight. Muscles that bring legs together into a sitting position are much tighter than the muscles that bring the legs apart and straight at the hips. This increased pull raises the risk for hip dislocations.
The biggest culprit, in my opinion, is the dreaded oculogyric crises. Our daughter would twist her arms and legs in a contracted position for long hours during these attacks. The doctors discussed how these dystonic movements might have had cumulative effects on her body. At such a young age, her hip joint may have become dislocated. Combined with the reasons above, her hip never had a chance to form once it was out of place.

Rylae-Ann traveled internationally to have hip surgery to correct her dislocated hip. (Courtesy of Richard E. Poulin III)
Correcting a dislocated hip
The first thing we did was look at her diet. We had been working on improving muscle tone, but we talked with our dietitian about better supporting her joint and bone development. Most meals included whole milk, yogurt, cheese, mozzarella, tofu, or salmon.
Scheduling hip surgery took some time. With COVID-19 restrictions, we could not operate immediately after discovering Rylae-Ann had a dislocated hip. We had to wait almost a full year until our appointment. Additionally, we would have to travel to meet with a pediatric orthopedic surgeon that we trusted. Although we were eager to treat as soon as possible, the surgeon reassured us that we could do this surgery any time before she walked, since treatment earlier in life is safer and more successful than treatment after a child is walking. She wasn’t experiencing pain, so we reluctantly waited.
After the surgeon performed an open reduction so that he could split her hip bone to extend outward to form a more natural shape, he added a bone graft for new bone to grow between the split he created. Pins were added, and then she was stitched up.
The surgery was only the tip of the iceberg regarding the challenges that followed. While she was still anesthetized after surgery, doctors covered Rylae-Ann in a body cast. It began at her chest and went to her ankle on the operated side while the other side ended above her knee. The crotch area was left open for a makeshift diaper. A wooden dowel was between the legs to help keep the cast from flexing inward. Maintaining this for several months after surgery is a whole other story shared by many other parents.
Once she was out of the cast, physical therapy began. The therapy helped break down the scar tissue and sensitivity that accumulates when the body is placed in a single position for so long. Even though her cast was off, she remained in the same position as if it was still on for a long time. Today, she seems to favor keeping her operated leg straight.
While Rylae-Ann sat and slept, we monitored her positions. Using the guidance of our surgeon about postoperative care, we were more mindful of how we positioned her. Sleeping was the best time to check on her, since she spent the longest time in those positions.

Physical therapy was necessary for Rylae-Ann after hip surgery and wearing a spica cast. (Courtesy of Richard E. Poulin III)
Preventing hip dislocation
If you are an AADC parent or caregiver reading this, then you have taken the first step: knowing your child is at risk due to their low muscle tone and immobility issues. You can then be more mindful of their positions. By applying what is known as postural management, the caregiver can be specific about how they move and place the body when lying down or sitting. Also, you can apply movements and stretches that support proper hip development. This has been useful in helping other immobile children with similar conditions such as cerebral palsy.
When talking with the surgeon later about what more we could have done, he noted that we may not have been able to do much. However, he did mention that some doctors and physiotherapists encourage compression garments to support proper hip placement and stabilization. He noted that more research was needed and that it may not provide much support in preventing hip displacement. I do think it is still worth discussing with your doctor, as my view is that every little bit counts and adds up over time.
***
Note: AADC News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of AADC News or its parent company, Bionews, and are intended to spark discussion about issues pertaining to aromatic l-amino acid decarboxylase deficiency.




Leave a comment
Fill in the required fields to post. Your email address will not be published.